Pressure ulcers or bedsores are a serious and frustrating complication for the paralysed, debilitated or comatose patient confined to a bed or wheel chair. These ulcers form when soft tissue is compressed between a bony prominence such as the ischium, sacrum or trochanter and a supporting structure such as the bed or wheel chair
The growing incidence of spinal cord injuries due to automobile accidents and increased numbers of debilitated geriatric patients admitted to hospitals have drawn more attention to the problem of pressure ulcer prevention and treatment.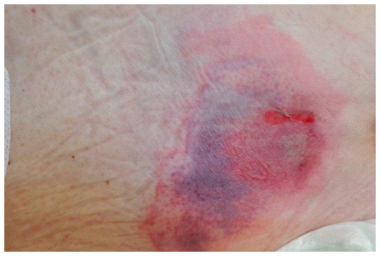
FACTORS PREDISPOSING:
Most important factor is pressure, other factors being paralysis, paresis, shearing forces, malnutrition, anaemia, advanced age and infection. Lack of protective sensation in comatose, debilitated patients, prevents them from changing posture. The localised pressure continues and skin ulcer develops. Initially there is tissue anoxia and cell death. Later active inflammation and vasodilatation occurs resulting in reactive hyperaemia.
CLINICAL FEATURES
- Early superficial ulceration • Erythema, oedema and punctate haemorrhage. Moist irregular ulceration with surrounding erythematous halo.
- Late superficial ulceration • Full thickness skin ulceration • Spreading necrosis of subcutaneous tissue • Deep inflammatory response spreads in cone-shaped fashion to deeper tissues.
- Late deep ulceration • Breakdown of fascia! plane • Chronic inflammation and fibrosis of deep tissue (bursa formation) There is no such thing as a small pressure ulcer. The visible skin wound is merely the "tip of the iceberg". 70% of the ulcer is below the skin. Pressure is transmitted in a coneshaped or pyramidal manner from the skin through each layer of tissue to the bony prominence, so that a cone of tissue destruction is created.
PREVENTIVE measures Pressure ulcers can be avoided by meticulous skin care and relief of pressure over bony prominence
TREATMENT:
- Superficial ulceration: Debridement and allowing it to heal by secondary intention. It will take many weeks to heal.
- 'Wet to dry' dressing
- Nutritional consideration
- Regular, periodical skin inspection, especially over the bony prominences.
HOMOEOPATHIC MANAGEMENT:
- Arnica: Arnica is the best homeopathic remedy for bed sores that have made the skin turn blue-black in appearance. This may also be accompanied by soreness, itchiness, and a feeling as if the bed is too hard to lie down on. Arnica helps reduce blue-black spots and also prevents the formation of pus.
- Apis Mellifica:Bed sores that are rose coloured and accompanied by a burning sensation and pain on the spot that worsens with touch can be treated with this homeopathic remedy. In such cases, the patient may also have a desire to uncover the affected limb or area to reduce the burning and pain.
- Carbo Veg:Bed sores formed in areas where the skin turns blue due to cold but where the skin simultaneously sweats excessively can be treated with homeopathic remedy carbo veg. This patient may also complain of itching that worsens with warmth and towards the evening. In some cases, it is the best homeopathic remedies for bed sores bleeding.
- Arsenic Album:Homeopathic remedies arsenic album used for bed sores problem. Ulcers that give off an offensive discharge can be treated with this homeopathic remedy. Such ulcers are often also quite painful and this pain worsens at night and with the cold. The person may also be weakened by the ulcers.
- Silica and Hepar Sulph:Bedsores that are filled with pus can be effectively treated with homeopathic medicine Silicea. In cases where this pus turns bloody, homeopathic remedy Hepar sulp prescribed to treat bed sores.


