

Pulmonary hypertension is a type of high blood pressure that affects the arteries in lungs and the right side of heart.
In one form of pulmonary hypertension, called pulmonary arterial hypertension (PAH), blood vessels in lungs are narrowed, blocked or destroyed. The damage slows blood flow through the lungs, and blood pressure in the lung arteries rises. Heart must work harder to pump blood through lungs. The extra effort eventually causes your heart muscle to become weak and fail.
In some people, pulmonary hypertension slowly gets worse and can be life-threatening. Although there is no cure for some types of pulmonary hypertension, treatment can help reduce symptoms and improve quality of life.
The signs and symptoms of pulmonary hypertension develop slowly. One may not notice them for months or even years. Symptoms get worse as the disease progresses.
Pulmonary hypertension symptoms include: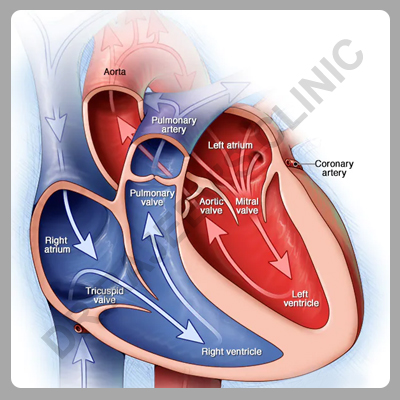
Heart has two upper chambers (atria) and two lower chambers (ventricles). Each time blood passes through heart, the lower right chamber (right ventricle) pumps blood to lungs through a large blood vessel (pulmonary artery).
In lungs, the blood releases carbon dioxide and picks up oxygen. The blood normally flows easily through blood vessels in lungs (pulmonary arteries, capillaries and veins) to the left side of heart.
However, changes in the cells that line your pulmonary arteries can cause the walls of the arteries to become stiff, swollen and thick. These changes may slow down or block blood flow through the lungs, causing pulmonary hypertension.
Pulmonary hypertension is classified into five groups, depending on the cause.
Causes include:
Causes include:
Causes include:

Causes include:
Causes include:
Eisenmenger syndrome is a type of congenital heart disease that causes pulmonary hypertension. It's most commonly caused by a large hole in heart between the two lower heart chambers (ventricles), called a ventricular septal defect.
This hole in heart causes blood to flow incorrectly in heart.Oxygen carrying blood (red blood) mixes with oxygen-poor blood (blue blood). The blood then returns to lungs instead of going to the rest of your body increasing the pressure in the pulmonary arteries and causing pulmonary hypertension.
Growing older can increase risk of developing pulmonary hypertension. The condition is more often diagnosed in people ages 30 to 60. However, idiopathic PAH is more common in younger adults.
Other things that can raise the risk of pulmonary hypertension include:
Complications of pulmonary hypertension include:
Right-sided heart enlargement and heart failure (cor pulmonale) - In cor pulmonale, our heart's right ventricle becomes enlarged and has to pump harder than usual to move blood through narrowed or blocked pulmonary arteries.
At first, the heart tries to compensate by thickening its walls and expanding the chamber of the right ventricle to increase the amount of blood it can hold. But these changes create more strain on the heart, and eventually the right ventricle fails.
Homeopathy is one of the most popular holistic systems of medicine. The selection of remedy is based upon the theory of individualization and symptoms similarity by using holistic approach.
Lachesis,Aurum Met,Aconite, Allium Cepa,Strophanthus,Nat. Mur, Plumbum Met, Carbo Animalis,Gelsemium, Ignatia,Glonine,Baryta Mur, Veratrum Viride,Belladonna,Arsenic Alb, Thuja, Adrenalin and many other medicines.
RL 18